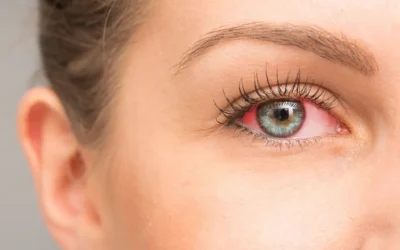
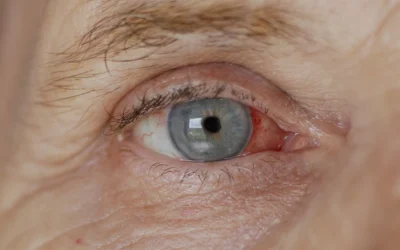
Dry, scratchy eyes can feel like they showed up overnight. One day you’re fine, and the next you’re blinking constantly, rubbing your lids, or feeling like there’s sand trapped under your contacts. Sudden dryness can be annoying, distracting, and even a little worrying, especially if you have existing eye health issues like glaucoma. While dry eye symptoms are often related to the surface of the eye (not the optic nerve), changes in medications, screens, seasons, and health conditions can trigger a flare that feels “all of a sudden.”
Below are the most common reasons for sudden dry eye and what you can do to feel comfortable again.
Why your eyes can turn dry so quickly
Your tears aren’t just “water.” They’re a layered mix of oil, water, and mucus that keeps vision clear and the eye surface protected. If any layer becomes unbalanced, symptoms can spike fast.
Common quick-change triggers include:
- Weather and indoor air: Cold wind, forced heat, fireplaces, and low humidity can dry the tear film within days.
- Screen time: Extra time on laptops or phones often reduces blinking, so tears evaporate faster.
- Contact lens wear: A new brand, longer wearing hours, or lenses past their replacement date can increase dryness.
- New medications or dosage changes: Antihistamines, antidepressants, acne medications, blood pressure medications, and some sleep aids can decrease tear production.
- Allergies: Seasonal allergies can cause inflammation that feels like dryness (and eye rubbing makes it worse).
Dry eye or something else?
It sounds backwards, but irritation from dry eye syndrome can trigger reflex tearing (excessive tears). Your eyes try to “flood” the problem, but that extra tearing is often poor-quality and doesn’t last.
Dryness may be more likely if you notice:
- Burning, stinging, or a gritty sensation
- Blurry vision that clears with blinking
- Light sensitivity
- Redness, especially late in the day
- Discomfort with contacts that used to feel fine
If you have sharp pain, significant light sensitivity, thick discharge, or a sudden drop in vision, it’s worth being evaluated promptly to rule out infection or other issues.
Health conditions that can trigger dry eye disease
Sometimes the “sudden” part is your body shifting in ways you can’t see. A few health-related causes we commonly consider:
- Hormonal changes (pregnancy, postpartum, perimenopause/menopause, thyroid conditions)
- Autoimmune disease (like Sjögren’s, rheumatoid arthritis, lupus)
- Eyelid inflammation (blepharitis) or oil gland blockage (meibomian gland dysfunction)
- Diabetes-related changes: Diabetes can affect nerves and tear production, and it can also be linked with diabetic eye disease, which is one reason comprehensive eye exams matter even if your main complaint is “just dryness.”
Dry eye relief beyond “just use drops”
Artificial tears can be useful, but it’s worth identifying the underlying pattern. A visit with an experienced eye doctor can help you determine the cause of your discomfort and a treatment plan tailored to your lifestyle.
Supportive options your eye doctor may recommend include:
- Preservative-free lubricating drops and gel/ointment at night
- Lid hygiene routines to calm inflammation and improve oil flow
- Warm compresses for meibomian gland dysfunction
- Prescription therapies that reduce inflammation and improve tear quality
- In-office treatments for longer-lasting relief
Feel comfortable again with a vision plan that fits your life
If your eyes are burning, gritty, watering, or blurring more often, schedule a comprehensive eye exam with Avon Vision Associates or New Hartford Eye Associates to get to the root cause and start a treatment plan that helps you see and feel better.